CREDENTIALED. ENROLLED. BILLING.
Fast, Reliable Medical Credentialing & Provider Enrollment. Without The Headaches
Medical credentialing and insurance enrollment shouldn't delay patient care or disrupt your revenue cycle. Yet most healthcare providers face credentialing delays, payer rejections, and compliance issues that slow down approvals and billing.
PayerReady pairs a dedicated credentialing specialist with a tracking dashboard. We prepare applications, submit to every payer on your list, follow up until approval, and track every license and certification expiration.
Used by solo practitioners, multi-provider groups, and health systems across all 50 states.
Credentialing workflows that move without you pushing
Secure, HIPAA-compliant document storage
License & compliance tracking with expiration alerts
ALL-IN-ONE CREDENTIALING
Complete provider credentialing & payer enrollment managed in one platform.
PayerReady manages provider credentialing for commercial insurance, government payers, and IPAs. Every application is validated against payer-specific requirements before submission, so your enrollments move through without stalling.
From individual providers to large multi-location practices, we centralize and manage every step: submission, follow-ups, contracting, and renewals.
Commercial Payer Enrollment
Get In-Network. Get Contracted. Get Paid Better.
Expand your patient base by securing memberships with top-tier commercial insurers like BCBS, UHC, Cigna, and Humana. PayerReady removes the administrative burden so you can focus on care while we focus on your contracts.
Zero-Defect Submissions
We manage the paperwork and follow-ups, ensuring your application moves through without stalling.
Higher Reimbursements
We review fee schedules during contracting and flag reimbursement rates that fall below your specialty benchmarks.
Never-Miss Maintenance
We automate your re-credentialing and demographic updates, protecting you from "provider not enrolled" denials.

Insurance Mappings
User Insurance List
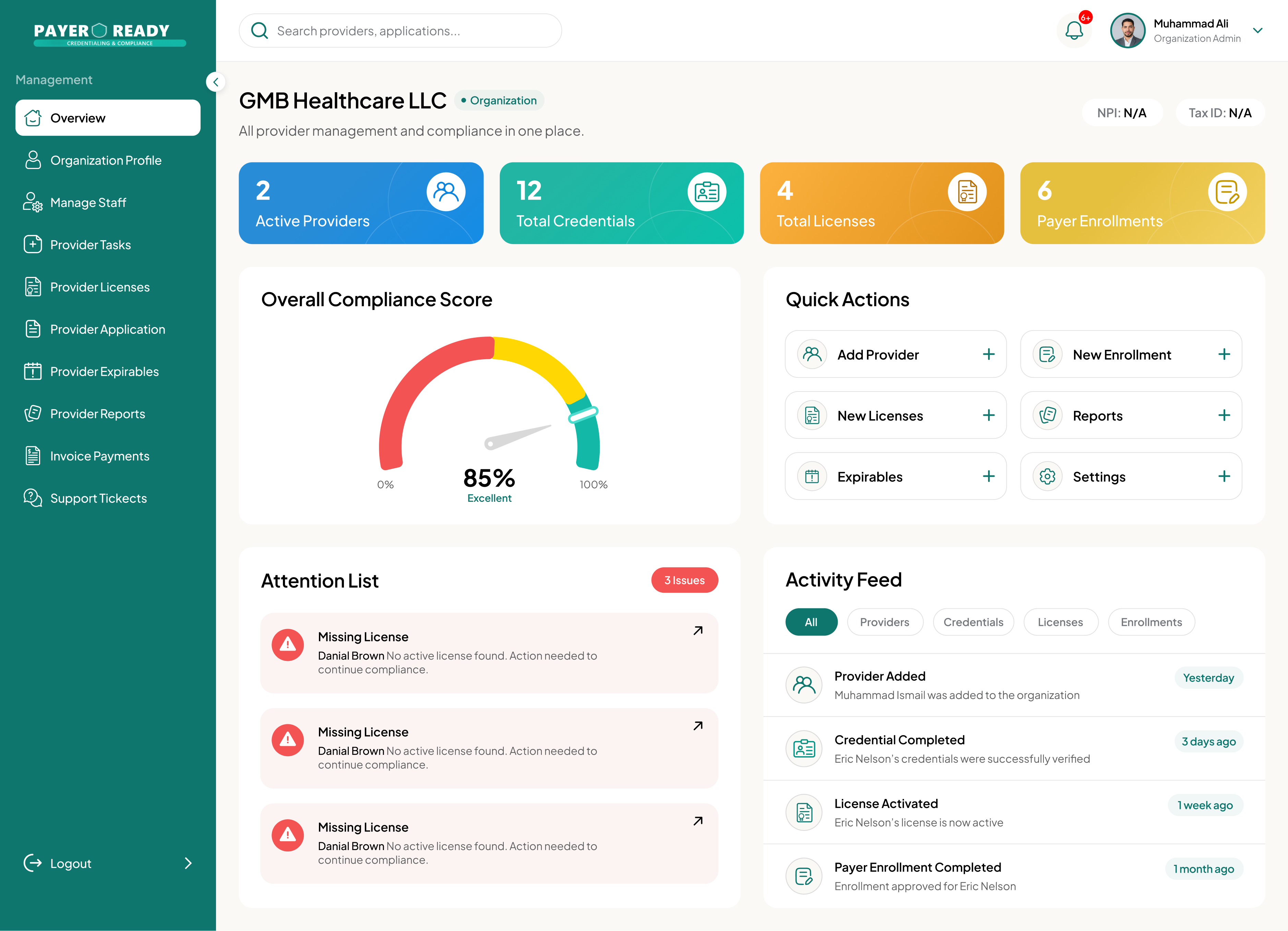


Government Insurance Credentialing
Federal and State Enrollment, Done Right the First Time.
Government payer enrollment is notoriously rigid. A single administrative oversight can result in months of "pending" status and deferred revenue. PayerReady provides the expert oversight needed to secure timely approvals for Medicare, Medicaid, and military health programs.
Medicare Enrollment (PECOS Integration)
We use the PECOS system to simplify your 855 applications and revalidations, reducing the risk of NPI deactivation.
State-Specific Medicaid Enrollment
Every state has a different portal, forms, and requirements. We know each one and handle the submissions so you don't have to figure out 50 different systems.
TRICARE & VA Healthcare
Expand your reach to veterans. We ensure accurate enrollment into the Community Care Network (CCN).
IPA (Independent Physician Association) Enrollment
Get Better Contract Terms & Higher Reimbursement Rates.
Joining an IPA gives your practice the collective bargaining power of a larger group, leading to better contract terms and a steady stream of patient referrals. PayerReady handles the entire IPA process, from initial application to ongoing compliance, so you get the network benefits without the paperwork.
Application Management & Primary Source Verification
We handle the heavy lifting of form submission and document verification to ensure your membership is processed without delays.
Strategic Contract Advocacy
Our team assists in the contracting phase, helping you secure the favorable reimbursement rates and incentive programs that IPAs offer.
Ongoing Compliance & Membership Renewals
IPA participation requires constant maintenance. We track your renewals and compliance milestones to ensure your status never lapses.
RELIABLE SOLUTIONS
Trusted Medical Credentialing Platform for
Healthcare Providers Nationwide
PayerReady supports healthcare organizations across multiple specialties and practice sizes.
Medical Practices
Physicians, specialists, nurse practitioners, urgent care centers, and multi-location clinics.
Dental Professionals
Dentists, orthodontists, and dental clinics seeking broader insurance participation.
Vision Care Providers
Optometrists and ophthalmologists aiming to maximize reimbursements.
Mental & Behavioral
Health Providers
Psychiatrists, psychologists, therapists, counselors, and behavioral health organizations.
EASY PROCESS
How PayerReady Works: Simple,
Secure, Transparent
Create a Free PayerReady
Account
No setup fees. No long-term contracts.
Submit Provider & Practice
Information
One secure intake used across all payers.
We Handle Credentialing &
Enrollment
Applications & compliance, fully managed
Track Credentialing Status
in Real Time
Full transparency from submission to approval.
Get Approved & Start
Billing Insurance
Activate contracts & increase revenue faster.
CREDENTIAL. APPROVE. EARN.
Faster Credentialing. Faster
Approvals. Stronger Revenue.
PayerReady replaces spreadsheets, shared drives, and manual follow-ups with a single dashboard and a dedicated specialist. Whether you're enrolling with commercial insurers, Medicare, Medicaid, or IPAs, every application is tracked from submission to approval.
Why Healthcare Providers Choose PayerReady
Less Admin Work. Faster Approvals. Full Compliance.
Reduce Administrative Burden
Eliminate repetitive paperwork and manual follow-ups.
Stay Continuously Compliant
Automated license, credential, and revalidation tracking.
Access Top Insurance Payers
Commercial and government networks made easy.
Fast-Track Credentialing Approvals
Fewer errors. Faster processing. Better cash flow.