Stop losing revenue
waiting on credentialing.
We get you approved faster—with full transparency and a 99.8% first-pass acceptance rate. Focus on patients, we'll handle the payers.
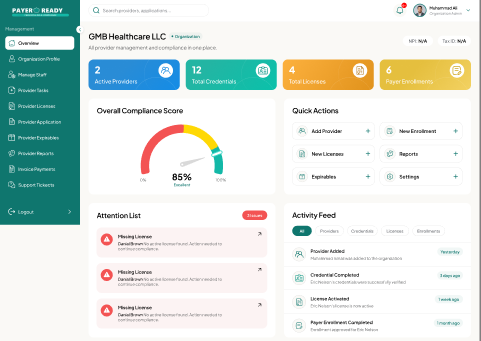
A Smarter Way to Manage Medical Credentialing
Healthcare credentialing is one of the most crucial yet complex processes for medical professionals. We've created credentialing software that will change how you credential forever.
The Credentialing Portal revolutionizes medical credentialing services by eliminating delays, reducing paperwork, and automating tedious processes.
Why Practices Choose PayerReady
We built PayerReady to solve the biggest headaches in provider data management and payer enrollment, simplifying complex workflows and reducing administrative burden.
Dedicated Specialist
One point of contact who manages the full credentialing process, start to finish for every provider.
Ready Applications
We prepare and package payer enrollments exactly as committees require—clean, compliant, and on time.
Proactive Follow-ups
No more wondering where things stand. We follow up relentlessly with payers until approval is complete.
Flexible Support
From solo providers to multi-state groups, our service scales with your practice's unique needs.
All-in-One Credentialing Platform
One platform to manage onboarding, credentialing, compliance, and provider operations—fast, secure, and always audit-ready.
Self-Service Client Onboarding Portal
Clients onboard themselves with guided steps and real-time tracking, reducing manual effort and ensuring accuracy.
Dedicated Credentialing Specialist
Each account is supported by a dedicated credentialing expert for accuracy, faster turn-around, and personalized support.
Automated Credentialing
End-to-end automation for payer credentialing and enrollments. Eliminates delays, rework, and manual follow-ups.
One-Click Applications & Renewals
Submit applications and renewals with a single click. Pre-filled data ensures speed and consistency.
EFT & ERA Enrollment Management
Manage EFT and ERA enrollments from one centralized platform. Streamlines payment and reconciliation processes.
Exclusion Monitoring & Verification
Continuous monitoring against federal exclusion databases. Protects practices from compliance risks.
Credentialing Made Easy
We simplify medical credentialing by reducing delays and rejections, while improving compliance and reimbursements.
High Rejection Rates & Delays
Compliance Challenges
Administrative Burden
Provider Directory Inaccuracies
Re-Credentialing
EFT & ERA Setup Issues
Out-of-Network & Enrollment Denials
High Rejection Rates & Delays
Reduce delays and paperwork by efficiently automating the credentialing process.
Benefits of Our Credentialing Portal
Our specialist-driven process delivers industry-leading results that directly impact your bottom line.
Save Time
Reduce delays and paperwork by automating the credentialing process.
Stay Compliant
Stay up-to-date with licensing and certifications compliance to avoid penalties.
Simplify Renewals
Reduce delays and paperwork by automating the credentialing process.
Reduce Admin Work
Optimize document management and administrative tasks, allowing you to focus on patient care.
Data Security
Protect sensitive information with HIPAA-compliant storage and end-to-end encryption.
From Kickoff to Approval in 4 Simple Steps
We've refined our end-to-end enrollment process to remove complexity, reduce delays, and give providers full visibility at every stage — from initial kickoff to final approval.
Get Started TodaySign Up
Create your account and gain immediate access to our secure provider portal.
Request Setup
Submit your provider details and practice locations with a few simple clicks.
Payer Enrollment
We manage the submission and relentless tracking of all your applications.
Approval & Go-Live
Approve your effective dates and start billing. We handle ongoing re-credentialing.
Our Expertise Includes
Network access issues and enrollment suspensions can disrupt your revenue. Our smart solutions quickly resolve payer restrictions to keep your operations running smoothly.
Credentialing Experts & Insurance Enrollment
Effortless enrollment with payers, ensuring timely approvals and network participation.
Contracting & Negotiations
Maximize reimbursements with strategic payer negotiations and optimized contracts.
Revalidation & Compliance Services
Stay compliant with automated tracking, renewal alerts, and regulatory support.
EDI & EFT Enrollment Services
Accelerate claim processing and payments with seamless electronic transactions.
Licensing & Signup
Simplify licensing applications, renewals, and provider signups across states.
Exclusions Management
Prevent risks with proactive monitoring and exclusion verificatio.
What Our Partners Say
Practices of all sizes trust PayerReady to accelerate revenue and eliminate administrative headaches.
Trackio completely streamlined our payroll and compliance processes. We now spend 70% less time on finance admin and I'm 100% more confident in our numbers.
As a solo provider, I don't have time for paperwork. PayerReady managed my entire enrollment for Medicare and the top 5 commercial payers.
We switched from spreadsheets and scattered workflows to a single source of truth. Trackio makes finance feel like a superpower.
The credentialing process used to take us months. With PayerReady, we're seeing approvals in weeks. It's a game changer for our revenue cycle.
As a solo provider, I don't have time for paperwork. PayerReady managed my entire enrollment for Medicare and the top 5 commercial payers. I was seeing patients and getting paid weeks sooner than I could have on my own.
The level of detail and proactive communication from their team is unmatched. Highly recommend for any growing medical practice.
Switching to PayerReady was the best decision we made this year. Our rejection rate dropped significantly.
PayerReady's portal gives us total visibility. We no longer have to guess the status of our applications.
The Trackio team really understands fintech. Their onboarding support and compliance tools saved us weeks.
We switched from spreadsheets and scattered data flows to a single source of truth. Trackio makes finance feel like a superpower.
Excellent service and support. They really go above and beyond to ensure our doctors are credentialed correctly.
PayerReady has saved our practice countless hours of administrative work. We can finally focus on patient care.
Stop Doing It the Hard Way
See how a dedicated specialist with PayerReady compares to the headaches of manual, in-house credentialing.
Frequently Asked
Questions
Answering your questions about our process, scope, and how we help practices like yours.
We are a first-of-its-kind, credentialing software that replaces the "Book a Demo" model with instant self-sign up. You get the speed of technology with the accuracy of a dedicated human specialist.
We are built for solo practitioners and small to medium-sized practices. Our transparent, self-service model ensures expert credentialing is affordable and accessible to providers of all sizes.
We work with all major Commercial Payers, Medicare, and Medicaid programs across the US. We handle specific state plans and local networks.
Absolutely. Our specialists are experts at correcting, verifying, and maintaining messy or incomplete CAQH profiles.
We initiate relentless, proactive follow-up contacts—often 20+ times—to eliminate payer bottlenecks.
Ready to Eliminate Credentialing Delays?
Answering your questions about our process, project scope, and the ways we help practices like yours streamline operations, save time, and maximize efficiency.